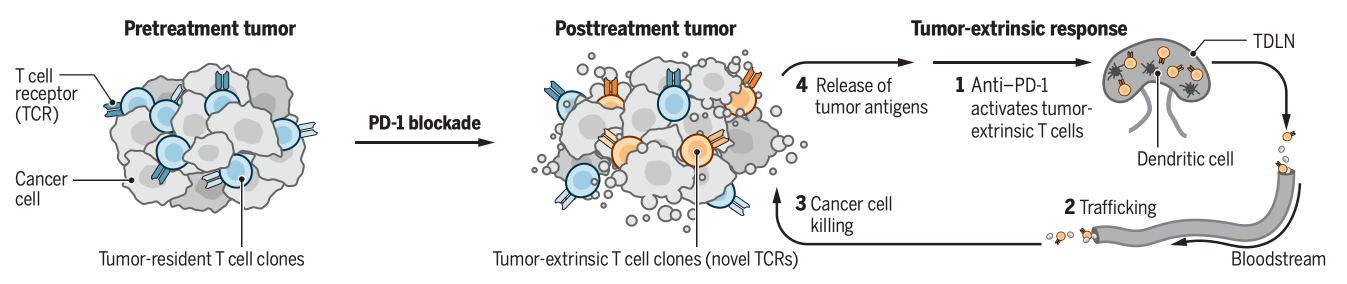
Immunotherapies that enhance the ability of the immune system to target cancer cells have proven effective in a variety of tumor types, yet clinical responses vary across patients and cancers. The most effective immunotherapies to date are immune checkpoint blocking antibodies, which target inhibitory surface receptors expressed by T cells, particularly programmed cell death 1 (PD-1). One of the few robust correlates of clinical response to PD-1 blockade is the presence of tumor-infiltrating T lymphocytes (TILs) prior to treatment, with immune-infiltrated tumors achieving better responses than “immunedesert” tumors (1). Therefore, it has been widely assumed that PD-1 blockade reinvigorates preexisting cells within the tumor microenvironment (TME). However, recent studies of T cell dynamics suggest that the T cell response to immune checkpoint blockade (ICB) may originate outside the tumor and rely on peripheral T cell recruitment. This has important implications for patient selection, predictive biomarkers, and design of combination treatment regimens.